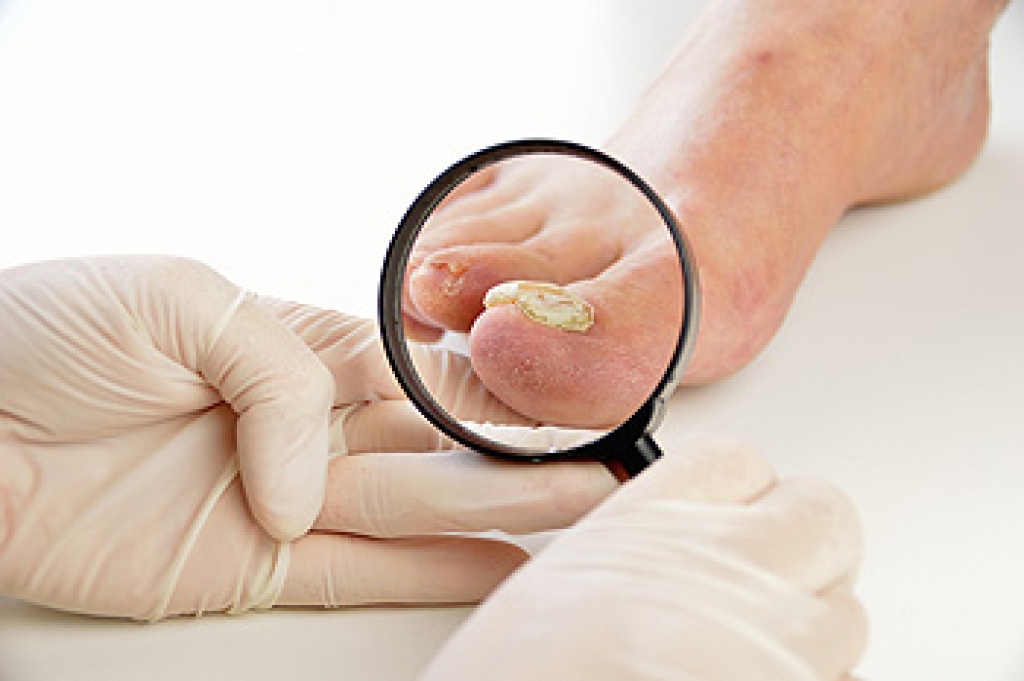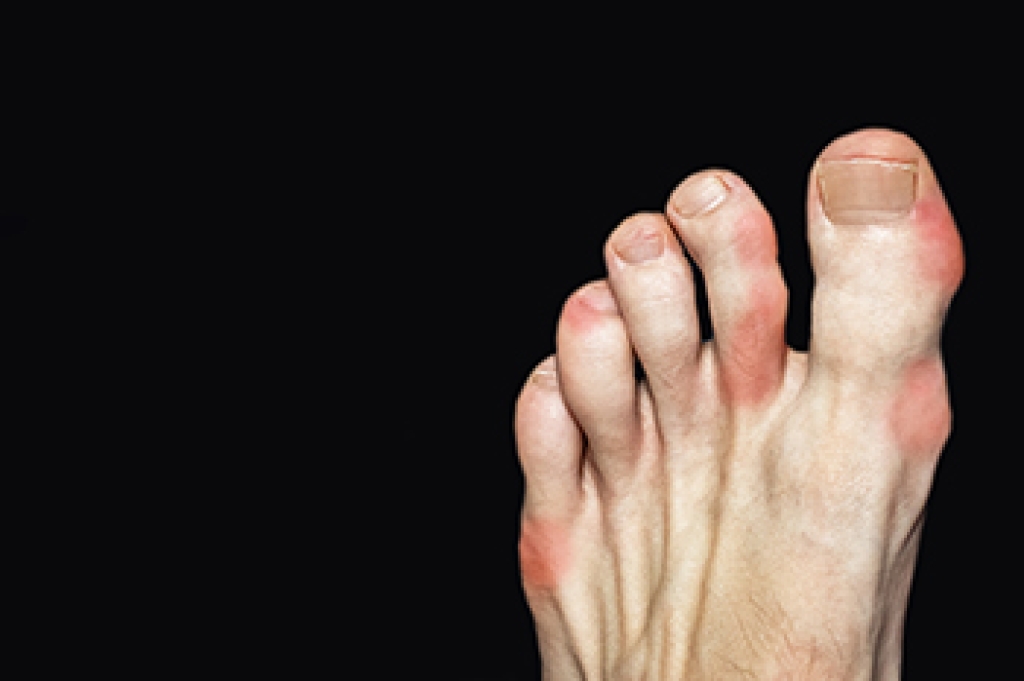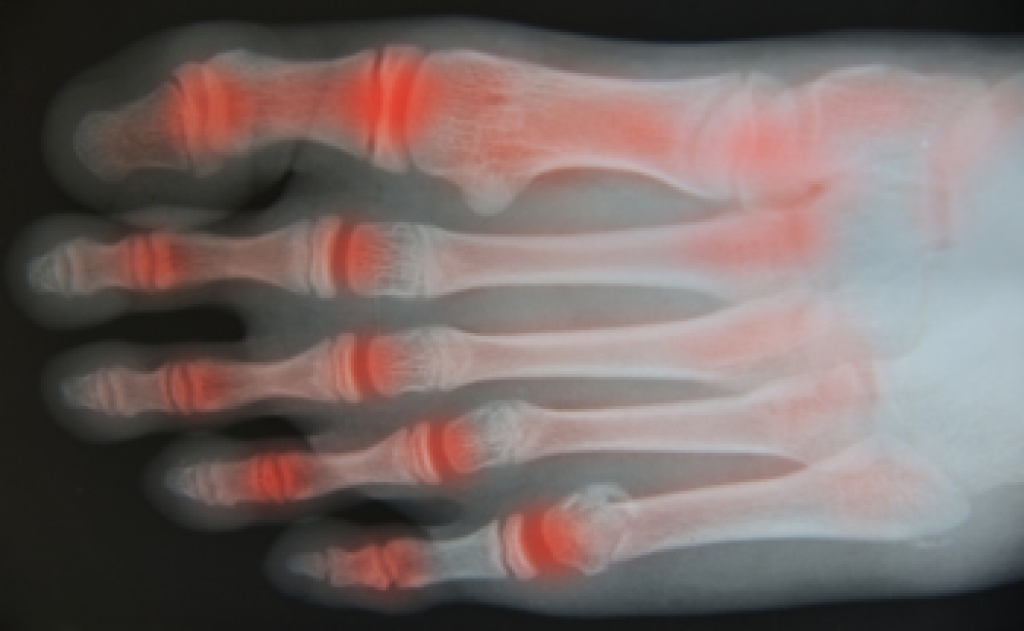
Foot arthritis is a condition that causes inflammation and joint damage in the feet, often leading to pain and limited movement. Osteoarthritis, or OA, develops over time as cartilage wears down, causing stiffness and aching that worsens with activity. Rheumatoid arthritis, or RA, is an autoimmune condition that leads to joint swelling, warmth, and deformity as the immune system attacks healthy tissue. Gout is a form of arthritis caused by a buildup of uric acid crystals, often creating sudden and intense pain, redness, and swelling in the joints. Each type can affect walking and daily comfort in different ways. A podiatrist can diagnose the specific type, provide imaging, and create a treatment plan to protect joint function and reduce pain. If you are experiencing joint pain in your feet, it is strongly suggested that you consult a podiatrist for proper evaluation and appropriate relief and management solutions.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Susan Yeager, DPM from Yeager Foot and Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a term that is commonly used to describe joint pain. The condition itself can occur to anyone of any age, race, or gender, and there are over 100 types of it. Nevertheless, arthritis is more commonly found in women compared to men, and it is also more prevalent in those who are overweight. The causes of arthritis vary depending on which type of arthritis you have. Osteoarthritis for example, is often caused by injury, while rheumatoid arthritis is caused by a misdirected immune system.
Symptoms
- Swelling
- Pain
- Stiffness
- Decreased Range of Motion
Arthritic symptoms range in severity, and they may come and go. Some symptoms stay the same for several years but could potentially get worse with time. Severe cases of arthritis can prevent its sufferers from performing daily activities and make walking difficult.
Risk Factors
- Occupation – Occupations requiring repetitive knee movements have been linked to osteoarthritis
- Obesity – Excess weight can contribute to osteoarthritis development
- Infection – Microbial agents can infect the joints and trigger arthritis
- Joint Injuries – Damage to joints may lead to osteoarthritis
- Age – Risk increases with age
- Gender –Most types are more common in women
- Genetics – Arthritis can be hereditary
If you suspect your arthritis is affecting your feet, it is crucial that you see a podiatrist immediately. Your doctor will be able to address your specific case and help you decide which treatment method is best for you.
If you have any questions please feel free to contact our office located in Redding, CA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.